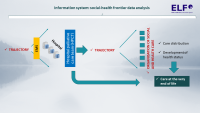
The organisation of end-of-life care is essential to the comprehensive provision of health services. Moreover, care for patients who can be expected to die predictably as a result of chronic disease is a demographically and epidemiologically growing segment of care. This is due both to the demographic ageing of the population and to the increasing success rate of treatment for many diseases that only 15 years ago significantly increased the mortality rate of the population (stroke, acute heart failure, cancer, etc.). The number of patients who will live to have more chronic diseases and significant polymorbidity in older age is thus steadily increasing.
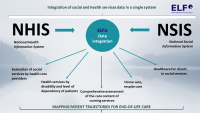
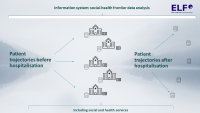
Palliative and end-of-life care is thus becoming a category of health services that requires predictive capacity planning, optimisation of the organisation of care, conceptual outcome evaluation and quality monitoring. From this perspective, this is not a simple segment, as comprehensive evaluation here requires a combination of many data sources. This is due, among other reasons, to the interdisciplinary nature of care, which involves a wide range of health service providers (ambulance services, primary outpatient care, hospital care) and health and social care at the end of the patient's life. At the same time, this is a segment of medicine that requires significant conceptual changes, as a large number of predictable deaths of chronically and terminally ill patients still take place in hospitals, in acute inpatient care. In addition to the fact that this essentially leaves no room for implementing the wishes of patients themselves and their relatives about the place of death, there is an overconsumption of health services through repeated hospital admissions at the end of life. The challenge for the management of this segment of medicine is thus to involve more significantly mobile palliative care, home care and, in general, health and social services provided in the natural social environment of the patient (client).
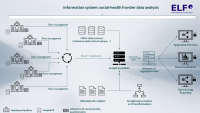
The reasons mentioned above inevitably increase the need for a high-quality and comprehensive data background for mapping and evaluating end-of-life care. The End of LiFe Care Information System (ELFis), which has been developed and implemented, aims to meet this need without building costly centralised data repositories or increasing the administrative burden of the system. The system's pilot testing and regional implementation, which is mainly based on the centralised data reporting already in place, has shown that such an information system is feasible. ELFis is a representative source of data and a comprehensive system for assessing the quality of this care segment.
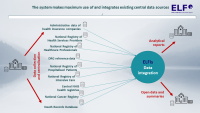
The design of the ELFis system was based on the conclusions and findings of the analytical phase of the “Palliatr Vysočina” project, which planned to collect the data needed to describe the issue of dying in terms of individual patient trajectories in the system, their quality of life, quality of care, previously expressed wishes and other attributes that stand outside the routine administration of health service provision. Unfortunately, the development of the project's delivery was severely disrupted by the COVID-19 epidemic, during which time it was impossible to implement advanced data collection or software solutions. However, this period and the virtual interruption of the project for almost three years paradoxically allowed a subsequent significant shift in the implementation of the assignment. This is because, during the COVID-19 epidemic, there was a substantial shift in the digitisation of health service evaluation; therefore, several data sources unavailable before 2020 are now automated by provider reporting (including primary outreach and outpatient clinics). Thus, it is no longer necessary to obtain these data through direct collection, which places a burden on clinical practice. Thus, the new ELFis system is a modern information system that maximises administrative reporting of provider data to central repositories and offers feedback and reporting in line with modern eHealth principles